You feel inflamed. Your joints ache. Your muscles are stiff. You're carrying extra weight you can't lose. Brain fog is constant. Fatigue never fully lifts. Your skin looks puffy. Your gut feels off.
Your doctor runs standard blood work. Everything comes back "normal." But you know something is wrong.
What you're experiencing is chronic inflammation—and it's measurable.
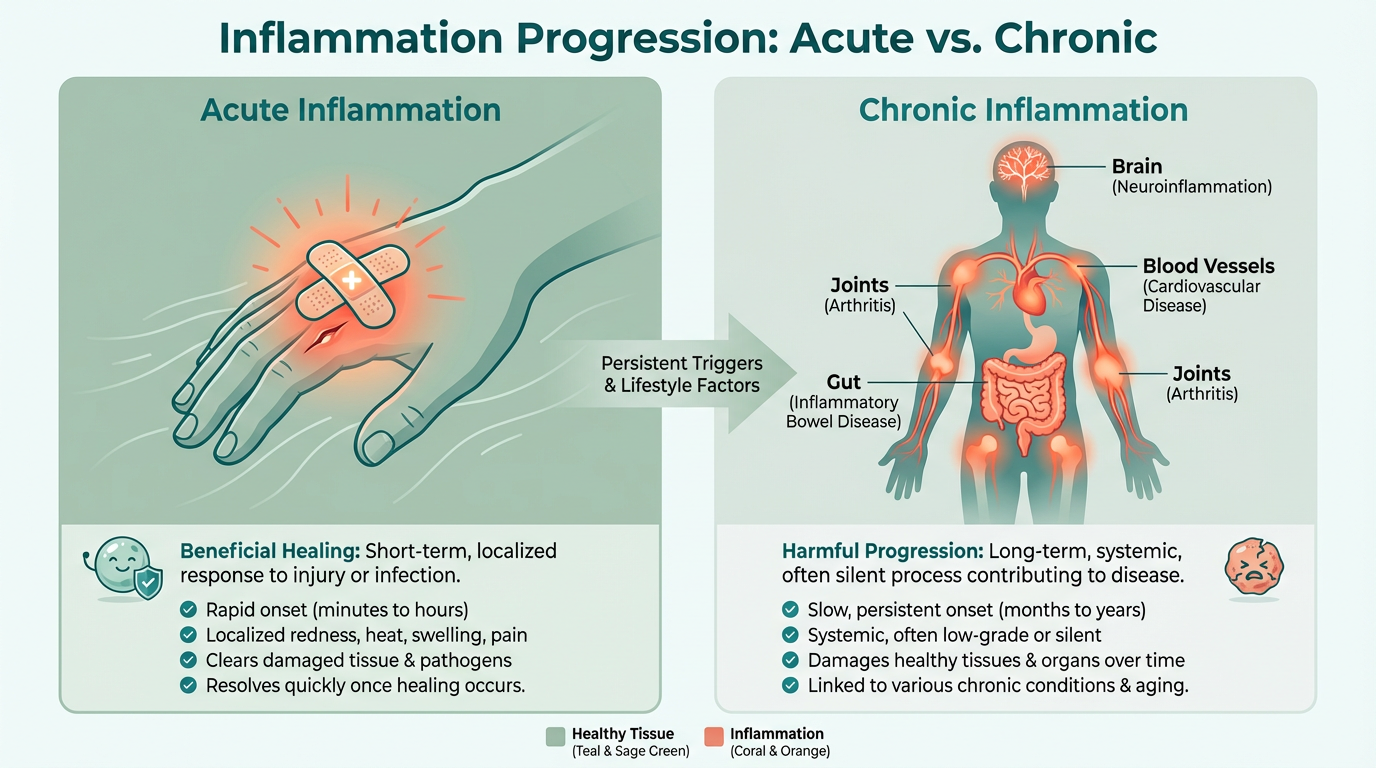
Acute vs. Chronic Inflammation: Why One Heals and One Destroys
Acute inflammation is your body's healing response. You cut your finger, it swells, gets red, and heals. That's inflammation working correctly—it's temporary, localized, and resolves when the injury is repaired.
Chronic inflammation is when that inflammatory response never turns off. It's systemic, low-grade, and persistent. It's your immune system constantly activated without a clear injury to heal.
The Key Difference
Acute Inflammation: Protective, short-term, localized
Chronic Inflammation: Destructive, long-term, systemic
Chronic inflammation is now recognized as the underlying driver of nearly every modern chronic disease:
- Heart disease
- Type 2 diabetes
- Alzheimer's and dementia
- Autoimmune conditions
- Cancer
- Depression and anxiety
- Obesity
- Chronic pain syndromes
If you're dealing with any of these—or if you just feel "inflamed" all the time—the root cause is often the same: chronic, systemic inflammation that's gone undetected.
What Causes Chronic Inflammation?
Chronic inflammation doesn't have one cause—it has multiple triggers working together. Think of it like kindling on a fire. One log might not keep the fire going, but when you keep adding more, the fire never goes out.
1. Diet (The Biggest Trigger)
The Standard American Diet is pro-inflammatory:
- Refined sugars and carbohydrates - Spike blood sugar and insulin, triggering inflammatory pathways
- Industrial seed oils (soybean, corn, canola) - High in omega-6 fatty acids, which promote inflammation
- Processed foods - Full of additives, preservatives, and chemicals your immune system sees as foreign
- Gluten and dairy (for sensitive individuals) - Can trigger immune reactions and gut permeability
2. Gut Dysfunction
Your gut lining is supposed to be a selective barrier. When it becomes permeable ("leaky gut"), undigested food particles, toxins, and bacteria leak into your bloodstream. Your immune system detects these as invaders and launches an inflammatory response.
Common gut triggers:
- Dysbiosis (imbalanced gut bacteria)
- SIBO (small intestinal bacterial overgrowth)
- Food sensitivities
- Chronic use of NSAIDs, antibiotics, or PPIs
3. Chronic Stress
Stress isn't just mental—it's biochemical. Chronic stress elevates cortisol, which initially suppresses inflammation but eventually causes cortisol resistance. Your cells stop responding to cortisol's anti-inflammatory signals, and inflammation runs unchecked.
4. Poor Sleep
Deep sleep is when your body repairs and clears inflammatory debris. When you're not getting quality sleep, inflammatory markers like CRP and IL-6 stay elevated. Even one night of poor sleep increases inflammation measurably.
5. Toxin Exposure
Your body is constantly filtering environmental toxins:
- Heavy metals (mercury, lead, cadmium)
- Pesticides and herbicides
- Plastics (BPA, phthalates)
- Mold and mycotoxins
- Air pollution
6. Insulin Resistance
High insulin levels directly promote inflammation. When your cells become insulin-resistant, your pancreas pumps out more insulin, creating a vicious cycle: insulin resistance → inflammation → more insulin resistance.
7. Chronic Infections
Low-grade infections you don't even know you have:
- H. pylori (stomach)
- Candida overgrowth
- Epstein-Barr virus (reactivated)
- Lyme disease and co-infections
- Dental infections (root canals, gum disease)
The Inflammatory Cascade
Trigger (diet, stress, toxins, gut dysfunction) →
Immune activation →
Cytokine release (TNF-α, IL-6, IL-1β) →
Chronic low-grade inflammation →
Tissue damage →
Disease
How to Test for Chronic Inflammation
You can't manage what you don't measure. Here's what we test:
1. High-Sensitivity C-Reactive Protein (hs-CRP)
The gold standard inflammatory marker. Produced by the liver in response to inflammation.
| hs-CRP Level | Status |
|---|---|
| <1.0 mg/L | Low inflammation (optimal) |
| 1.0–3.0 mg/L | Moderate inflammation |
| >3.0 mg/L | High inflammation (heart disease risk) |
2. Other Key Markers:
- ESR (Erythrocyte Sedimentation Rate) - Measures how fast red blood cells settle
- Homocysteine - Elevated indicates inflammation and oxidative stress
- Ferritin - Iron storage protein that rises with inflammation
- Fasting Insulin - High insulin = inflammation
- Omega-3 Index / AA:EPA Ratio - Measures pro-inflammatory vs anti-inflammatory fat balance
How to Turn Off Chronic Inflammation
Once we know your inflammatory markers and triggers, we build a systematic plan:
1. Remove Inflammatory Triggers
Diet:
- Eliminate refined sugars, seed oils, and processed foods
- Consider removing gluten and dairy for 30 days
- Eat whole, nutrient-dense foods: vegetables, quality proteins, healthy fats
Gut Healing:
- Test for dysbiosis, SIBO, parasites, or gut infections
- Support with probiotics, digestive enzymes, and gut-lining nutrients (L-glutamine, zinc carnosine, collagen)
Reduce Toxin Exposure:
- Filter your water
- Choose organic produce (especially for the "Dirty Dozen")
- Avoid plastic containers (use glass)
- Use non-toxic cleaning and personal care products
2. Add Anti-Inflammatory Support
- Omega-3 fatty acids (EPA/DHA) - 2–3 grams daily from high-quality fish oil
- Curcumin (with black pepper or liposomal form) - 1,000–2,000 mg daily
- Resveratrol - Antioxidant and anti-inflammatory compound
- Vitamin D - Immune-modulating (aim for 50–80 ng/mL)
- Magnesium - Calms the nervous system and reduces inflammatory cytokines
- SPMs (Specialized Pro-Resolving Mediators) - Advanced omega-3 metabolites that actively resolve inflammation
3. Optimize Sleep and Stress
- 7–9 hours of quality sleep nightly
- Morning sunlight exposure (sets circadian rhythm)
- Evening wind-down routine (no screens 1–2 hours before bed)
- Stress management: breathwork, meditation, nature time
4. Move Your Body (But Don't Overdo It)
Moderate exercise is anti-inflammatory. Overtraining is pro-inflammatory. Find the balance:
- Walking, swimming, cycling
- Resistance training (not to exhaustion)
- Yoga, stretching, mobility work
5. Support Detoxification
Help your body clear inflammatory debris:
- Hydration - Half your body weight in ounces of filtered water daily
- Sauna - Promotes sweating and toxin clearance
- Liver support - Milk thistle, NAC (N-acetylcysteine), glycine
Inflammation Reversal Timeline
2–4 weeks: Inflammatory foods removed, gut healing begins
4–8 weeks: CRP and inflammatory markers start dropping
3–6 months: Symptoms improve—less pain, more energy, clearer thinking
6–12 months: Full inflammatory reversal in most cases
Why We Test and Retest
Inflammation is invisible until you measure it. You might feel better, but we want to see the data: CRP dropping, homocysteine normalizing, ferritin coming down, insulin sensitivity improving.
Retesting after 3–6 months confirms the protocol is working—and guides adjustments if it's not.
Ready to Identify and Reverse Your Inflammation?
Let's test your inflammatory markers, identify your triggers, and build your anti-inflammatory protocol.
Schedule Your Free Discovery Call